Living with recurring infections in warming Sunderbans

Living with recurring infections in warming Sunderbans
Rising heat, floods and saline water are accelerating antimicrobial resistance in the Sundarbans, where women face repeated infections, harsher treatment and lasting health consequences.
24 Paraganas, West Bengal: “The lower abdominal pain was so severe that I couldn’t walk straight,” said Rama Baidya (47), sitting outside her home in Laskarpur village of Jharkhali gram panchayat in West Bengal’s South 24 Parganas district. “No antibiotics worked.”
For nearly five years, Baidya was treated repeatedly for urinary tract infections and bacterial vaginosis. Each course of antibiotics brought temporary relief, only for the infection to return, often more painful than before. As the medicines grew stronger, her recovery grew slower. By 2023, doctors told her there were no options left. Baidya underwent a hysterectomy.
The surgery cost her family Rs 25,000, including Rs 18,000 for the operation alone. Recovery took months. More damaging was what followed: Baidya could no longer do the labour-intensive work that had sustained her family for over a decade after the hysterectomy.
For 15 years, Baidya and her husband earned a living by fishing, catching crabs and prawns, and collecting meen, or prawn seedlings, from the rivers and creeks of the Sundarbans. During gon mukh—the days following the seventh and eleventh nights of the lunar cycle—she would wade into brackish waters at dawn to collect prawn seeds that were later sold to hatcheries. After the surgery, she was unable to return to the rivers. She lost nearly eight months of work even before the operation, and has had none since.
Like many women in the Sundarbans, Baidya had lived for years with recurring urinary tract infections and bacterial vaginosis, which later progressed to pelvic inflammatory disease. Antibiotics offered temporary relief, but the infections kept returning, often requiring stronger doses.
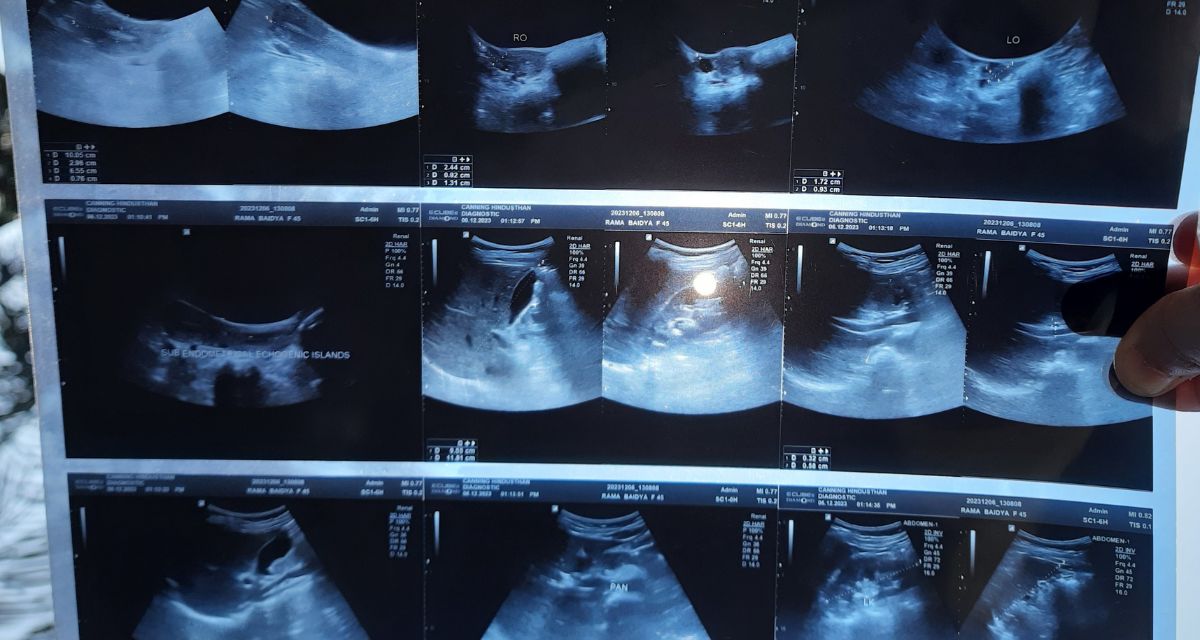
Doctors offered conflicting advice. One said the condition could still be managed with medicines. Another said surgery was the only option left. By the time Rama reached a private hospital in Canning, an ultrasound showed adenomyotic changes, an abnormal thickening of the uterine wall. Doctors explained that while adenomyosis does not directly result from urinary or vaginal infections, chronic pelvic inflammation and repeated infections can aggravate symptoms and complicate treatment, especially when infections stop responding to antibiotics. With her pain worsening and no antibiotic working anymore, she consented to the operation.
Baidya’s story reflects a wider, largely invisible public health crisis unfolding in the Sundarbans, where antimicrobial drugs that once treated common infections are increasingly failing—particularly among women.
In the Sundarbans, women spend long hours immersed in saline, flood-prone waters, fishing, collecting prawn seeds, or washing clothes. Clean and potable water is scarce. Cyclones, floods and tidal surges routinely contaminate ponds and shallow groundwater, disrupting sanitation and spreading pathogens. These conditions, doctors and researchers say, are accelerating infections and weakening the effectiveness of antimicrobial drugs used to treat them.
Antimicrobial resistance, or AMR, occurs when bacteria and other pathogens no longer respond to medicines designed to kill them. In the Sundarbans, doctors and paramedics say this resistance is becoming harder to ignore. Recurrent infections now take longer to heal, require higher doses, or demand stronger drugs that were once reserved for severe cases.
Nearly 60% of women in the region suffer from recurring urinary, reproductive or skin infections, health workers estimate. For years, antibiotics offered relief. Now, many women say they no longer do.
“The conditions that drive AMR here are deeply tied to climate stress,” said Dr Silvia Bertagnolio, unit head in the Antimicrobial Resistance Division at the World Health Organization, in an email response to 101Reporters. “Climate change creates warmer, more contaminated environments that accelerate the evolution of drug-resistant pathogens and weaken community health resilience, resulting in harder-to-treat infections and longer recovery times.”
Moreover, studies suggest that increasing global temperature is closely linked to AMR, because increasing temperatures lead to fast multiplication of pathogenic bacteria, more resistant in nature.
According to health workers in the Sundarbans, a growing number of women now require repeated and stronger antibiotic courses for common infections such as UTIs, bacterial vaginosis and skin diseases.
Where infection is hard to avoid
Women who collect prawn seeds in the Sundarbans spend long hours neck-deep in brackish rivers and creeks, dragging nets through mud and water. Many begin work as early as 2 am and return only by morning. During gon mukh, some travel deep into forested waterways, spending days or even weeks on boats to collect prawn seeds.
“When we are on the boat, our bodies, especially the lower part, remain soaked in brackish water all the time,” said Fularani Mondal of Pakhirala village in Gosaba. “There is no way to escape it.”
The hatcheries where prawn seeds are sold routinely add antibiotics to water tanks to prevent bacterial infections, said Bhakta Mondal, a resident of Jharkhali whose family members work in fisheries. While the antibiotics are not ingested through the prawns, workers—many of them women—are in constant contact with treated water during long shifts. Researchers warn that such repeated exposure can increase the presence of drug-resistant bacteria in aquatic environments, posing health risks to people who work in and around hatcheries.
Many bacteria found in aquatic environments are also capable of infecting humans. Exposure to antibiotics in hatcheries, researchers warn, can make these pathogens more resistant, posing risks to people who work in and around such environments.
Even women whose livelihoods are not directly tied to fishing face frequent infections. Most households depend on ponds for bathing and washing clothes, but clean water is scarce. After cyclones and floods, saline water routinely inundates villages across Patharpratima, Gosaba and Satjelia, contaminating ponds and shallow groundwater. Flooding disrupts sanitation and spreads microbes from human and animal waste into water sources, accelerating the spread of infections, including drug-resistant ones.
“AMR is making treatment increasingly difficult,” said Gouranga Sarkar, a paramedic from Jharkhali. “Patients with urinary, reproductive and skin infections now need longer recovery periods and higher doses of medicine.”
For many women, repeated treatment failures carry long-term consequences. “Some women choose hysterectomy at a very young age when antibiotics stop working,” said Anamika Mondal (30), a resident of Pakhirala Gram Panchayat. “It affects their intimate lives and overall wellbeing.”
Piya Hait (20), a homemaker from Patharpratima block, has struggled with recurring urinary and reproductive infections. Antibiotics and antifungal medicines offered brief relief, but symptoms returned soon after each course. “As soon as I finished the medicines, the problem came back,” she said. “It has changed my relationship with my husband forever.”
Diagnosed with thalassemia, which weakens immunity, Hait now avoids treatment unless her condition worsens. “The medicines are expensive,” she said. “I’ve stopped going to doctors. I don’t even know whom to talk to anymore.”
Others have been forced to give up work altogether. Kajal Mondal (52), from Pakhirala village, stopped collecting meen after years of recurrent infections. “My urinary infections improved after I stopped fishing,” she said, showing rashes on her hands. “But skin infections have become worse. This year, it’s unbearable.”
Health workers say many women now depend on higher doses of antimicrobial drugs than before, while others abandon treatment entirely.
In most places of the Sundarbans, the public health centres are distantly located. Most of the PHCs lack adequate health infrastructure or expert doctors, as reported by the locals. Villagers often travel miles and cross rivers through ferries to avail basic health services.
For sisters Chameli and Kuheli Mondal (names changed), students of Classes 8 and 12 from Pakhirala village in Gosaba, the impact is already visible. Recurrent urinary infections, bacterial vaginosis and painful menstrual cycles make it difficult for them to concentrate in school.
“Next year, Kuheli will appear for her board exam,” said their mother, Champa Mondal (name changed). “But with her repeated health problems, she has to travel 30 kilometres just to reach an examination centre.”
The family depends entirely on fishing, and their meagre income makes regular treatment difficult. Though the primary health centre in Gosaba is not far from Pakhirala, Champa said access to care remains poor.
“The doctors barely listen to us,” she said. “They write a prescription before we even finish explaining what we are going through.”
When no medication is strong enough
Doctors in the Sundarbans told 101Reporters that they are increasingly forced to prescribe stronger drugs—and higher doses—as common infections fail to respond to standard treatment.
“We do not track antimicrobial resistance, so it’s difficult to provide data-based insights,” said Dr Mahmud Hasan Shah, Block Medical Officer of Health at Madhabnagar Grameen Hospital in Patharpratima. “But in practice, we are seeing more treatment failures.”
When first-line drugs no longer work, he said, doctors move to broader-spectrum antibiotics which are effective against a wide variety of bacteria, used when cause of infection is unknown or multiple germs are suspected.
Private practitioners report similar trends. “So far, we haven’t observed resistance to it…but the concern remains,” said Dr Arpita Sarkar, a general medical practitioner in Patharpratima.
“Earlier, a 500 mg dose of levofloxacin(antibiotic) was sufficient for UTIs,” said Satyajit Hazra, a doctor based in Madhabnagar. “Over the past two to three years, that dose has stopped working for many patients. We now prescribe 750 mg to clear the infection.”
Antibiotics alone are no longer enough. “We now prescribe antifungals and even antivirals along with antibiotics,” said Dr Shah. Gouranga Sarkar, a paramedic from Jharkhali, added that doses of antifungal drugs have also increased. “Earlier, a week-long course was enough. Now, higher doses are needed.”
Despite these changes, recovery times are lengthening. “Infections are taking longer to heal,” said both Dr Sarkar and Gouranga Sarkar.
Not all frontline health workers report the same pattern. Aloklata Chatterjee, Nodal Medical Officer of Rangabelia Gram Panchayat, and Hemali Mondal, an ASHA worker from Satjelia, said fewer women report UTIs or bacterial vaginosis at their centres, which they attribute to awareness campaigns. However, both confirmed a noticeable rise in skin infections this year.
Women in several villages told a different story. Many said they rely on unqualified practitioners or stop seeking treatment altogether, either because public health centres are far away, or because they feel unheard. In places where clean water remains scarce, infections continue to recur.
Doctors and researchers said that climate stress is intensifying these trends.
“Increased heat and humidity create ideal conditions for drug-resistant microbes to multiply,” said Dr Bipin Adhikary, an infectious disease specialist at the University of Oxford. “Floods and cyclones further spread these pathogens, especially in low- and middle-income settings with weak health infrastructure.”
In 2024, global average temperatures crossed 1.5°C above pre-industrial levels. In West Bengal, the summer of 2025 brought early and intense heat, with temperatures repeatedly crossing 40°C, followed by prolonged monsoon rainfall. “This year, infections are taking much longer to recover from,” said Dr Sarkar. “The hot, humid conditions have been perfect for resistant pathogens.”
A 2022 study by scientists at Sun Yat-sen University in China found that even a 1°C rise in average temperature can significantly increase antimicrobial resistance in pathogenic bacteria. Health workers in the Sundarbans say the effects are already visible.
“The rise in skin infections this year is directly linked to extreme rainfall and a prolonged monsoon,” said Chatterjee. Gangetic Bengal, including South 24 Parganas, recorded repeated heavy rainfall events through the season, creating conditions where infections spread faster and medicines work slower.
Climate stress and women’s bodies
In the Sundarbans, antimicrobial resistance does not operate in isolation. The intersection of biological, socio-cultural, and economic factors—combined with inequity and gender disparity—drives the spread of infectious diseases and AMR-related complications. These same factors heighten women’s vulnerability to climate change.
Women are biologically more susceptible to infections affecting the urinary or genital tracts. In low- and middle-income regions like the Sundarbans, that vulnerability is intensified by poor sanitation, limited access to clean water, weak health infrastructure and entrenched gender inequality.
“Gender influences people’s exposure to infections, how they prevent them, and whether they seek timely care or attempt self-treatment,” Anand Balachandran, who heads National Action Plans at the World Health Organization’s AMR division, noted in a recent report.
In the Sundarbans, women shoulder both economic and domestic labour. Many continue working in rivers, fields and forests even when unwell, because illness does not pause hunger.
“My abdominal pain, heavy discharge and burning while urinating break me from inside,” said Sudha Patra (38) from Bhagbatpur village in Patharpratima. “But the men at home don’t understand. I still have to fish, collect meen or work in the paddy fields.”
For many women, stigma compounds neglect. Reproductive infections remain difficult to discuss, even within families. Seeking care is harder still when public hospitals are far away and staffed mostly by male doctors.
No clean cure
Global health agencies acknowledge the scale of the problem. A World Health Organization report published in October 2025 called for urgent strengthening of AMR surveillance, warning that resistant infections are rising faster than health systems can respond. While India contributes data to the WHO’s Global Antimicrobial Resistance Surveillance System, the report flagged large regional gaps and noted that most national AMR plans fail to account for gender and equity.
At the local level, frontline health workers offer basic advice. “We tell women to wash their urogenital area with clean water after urination and to bathe regularly to prevent infections,” said Aloklata Chatterjee and Hemali Mondal, health workers in Gosaba.
But largely, even that advice is impossible to follow.
“Clean water itself is a struggle,” said Anamika Mondal from Pakhirala village. “We walk miles every day just to collect drinking water. How are we supposed to use clean water to wash ourselves?”
This project is supported by the Internews Earth Journalism Network with funding from the Swedish International Development Cooperation Agency (Sida)
Cover image - In the Sundarbans, women keep fishing, farming prawns, or working in the paddy fields—despite the unrelenting pain of UTIs and PIDs, making them even more exposed to pathogenic microbes (Photo - Madhurima Pattanayak, 101Reporters)
Would you like to Support us
101 Stories Around The Web
Explore All NewsAbout the Reporter
Write For 101Reporters
Would you like to Support us
Follow Us On

 Women in the Sundarbans spend hour after hour in shoulder-deep brackish water to catch prawns, crabs, and meen (prawn seeds); In tiger prawn hatcheries, like the one above in Jharkhali, antibiotics are used to protect the meen from bacterial infections. Spending six to eight hours a day in this waist-deep muddy water exposes the women to antibiotic residues that heighten their risk of AMR (Photos - Madhurima Pattanayak, 101Reporters)
Women in the Sundarbans spend hour after hour in shoulder-deep brackish water to catch prawns, crabs, and meen (prawn seeds); In tiger prawn hatcheries, like the one above in Jharkhali, antibiotics are used to protect the meen from bacterial infections. Spending six to eight hours a day in this waist-deep muddy water exposes the women to antibiotic residues that heighten their risk of AMR (Photos - Madhurima Pattanayak, 101Reporters) 
 A health and wellness centre in Ramganga Gram Panchayet, Patharpratima Block (Photo - Madhurima Pattanayak, 101Reporters)
A health and wellness centre in Ramganga Gram Panchayet, Patharpratima Block (Photo - Madhurima Pattanayak, 101Reporters)  Three generations of women from a fishing family (the grandmother of the family, her daughter-in-law, and her granddaughter) from Pakhirala village suffer from UTI, PID, and skin infections (Photo - Madhurima Pattanayak, 101Reporters)
Three generations of women from a fishing family (the grandmother of the family, her daughter-in-law, and her granddaughter) from Pakhirala village suffer from UTI, PID, and skin infections (Photo - Madhurima Pattanayak, 101Reporters) 